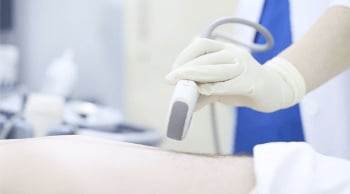
Normal Colour Doppler Flow Appearance of an AAA After Endovascular Repair (EVAR)
Ultrasound is key for assessing abdominal aorta post-EVAR, focusing on residual sac size, detecting endoleaks, and ensuring stent-graft patency. Learn the importance of color Doppler in EVAR evaluation.
Feb. 4, 2020 / ABC Vascular staff
Ultrasound is routinely used to assess the abdominal aorta after endovascular repair (EVAR) of an aortic aneurysm (AAA).
The main objectives of ultrasound assessment are:
- Detect variation in the AAA residual sac size
- Detect endoleaks
- Assess patency of the stent-endograft used to treat the AAA
While B-mode is mostly used to determine the maximum diameter of the residual AAA sac, colour Doppler flow plays a crucial role in detecting endoleaks and determining stent-graft patency. This short summary will illustrate the normal colour Doppler flow appearance of an EVAR.
Related ABC Vascular Courses
Have you considered learning more with these related courses?
Master course on Abdominal Aortic Aneurysms (AAA)
Info on the “Abdominal Aortic Aneurysm” course >
Short course on screening for AAA during Transthoracic Echocardiography
More on the “Screening for AAA During TTE” course >
Stent-Graft Patency
The aortic stent-graft needs to separate blood flow and pressure from the aneurysm wall so to prevent aortic aneurysm rupture. When colour Doppler flow is applied, therefore, colour should only appear throughout the stent-graft. The stent-graft will appear with colour filling its entire lumen (Figure 1). In order to obtain a good colour Doppler flow filling, an adequate colour pulse repetition frequency (PRF) and colour flow gain are essential. Generally, it is advisable to start the colour flow Doppler assessment with a low pulse repetition frequency (PRF), typically at 23 and then adjust this according to the ultrasound findings. If there is poor colour Doppler flow filling of the stent-graft, it is possible to further reduce the PRF and/or to increase the colour Doppler flow gain.
When a low PRF is used, attention should be paid to avoid colour Doppler flow bleeding artefact. Colour bleeding within the thrombosed AAA sac may mimic an endoleak thus causing a false positive diagnosis for the presence of an endoleak. Colour Doppler flow should therefore be observed only within the stent-graft placed through the entire length of the AAA and through the common iliac arteries when this are treated.
“Colour Doppler flow should be observed only within the stent-graft placed through the entire length of the AAA.”
Endoleak
Any blood flow (colour Doppler flow) seen within the aneurysm sac (between the native aortic wall and the wall of the stent-graft) is considered an endoleak and is classified according to its origin in accordance with previously published criteria 1.
To summarise, there are 5 types of endoleaks:
- Type I: incomplete seal at the proximal (a) or distal (b) seal zone
- Type II: Retrograde arterial branch flow from (a) inferior mesenteric artery or (b) lumbar arteries
- Type III: Incomplete seal between components, component separation, fabric erosion, or tear
- Type IV: Leak due to fabric porosity (generally only present at the time of operation)
- Type V: Endotension, sac enlargement without obvious endoleak (uncommon with current grafts)
If any of these leaks are present, colour Doppler flow will be shown outside of the stent-graft wall in different locations of the residual AAA sac.
“Any blood flow seen within the aneurysm sac (between the native aortic wall and the wall of the stent-graft) is considered an endoleak.”
As some types of endoleaks may involve the superior landing zone of the stents-graft and/or the distal sac of the AAA, it is advisable to assess the whole length of the treated AAA and common iliac arteries, in case these are treated too, for the presence of colour Doppler flow.
Although colour duplex ultrasound scan is the most widely used imaging modality for endoleak detection, its sensitivity and specificity in detecting endoleaks is lower when compared with CTA.
Contrast-enhanced ultrasound (CEUS) can be of help for further increasing the examination’s sensitivity, helping to find small endoleaks and to characterize their sources.

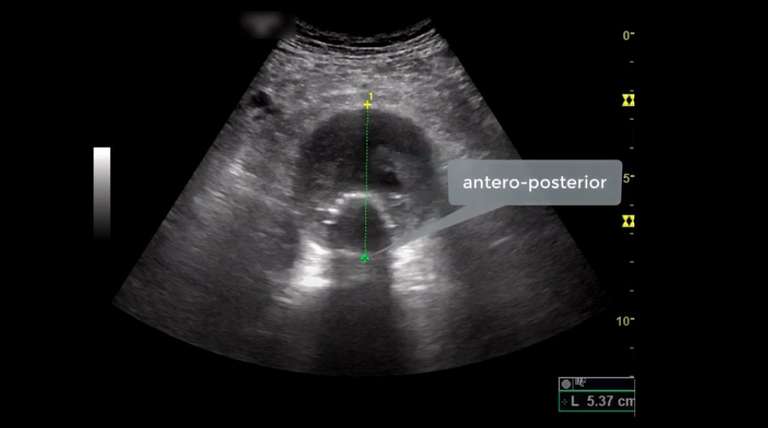
Figure 1 Description: Normal colour Doppler flow appearance of an EVAR, transverse view. The colour flow is noted only within the stents-endograft (*). A colour PRF of 23 is used. No colour flow is noted within the AAA sac size (between the stents and native walls of the abdominal aorta). The abdominal aorta lies above the Vertebral Body (VB) which is one of the main anatomical landmarks used to identify the abdominal aorta.
Reference
Bryce, Y., et al. 2015. Endovascular Repair of Abdominal Aortic Aneurysms: Vascular Anatomy, Device Selection, Procedure, and Procedure-specific Complications. Radiographics 35(2): 593-615.
Pubmed
Article link and further related Pubmed articles
Pubmed >