Assessment of Carotid Arterial Plaque
Discover the latest ASE recommendations on using ultrasound to assess carotid plaque for atherosclerosis characterization and cardiovascular risk evaluation.
Oct 30, 2020 / Dr. Cristiana Vitale & ABC Vascular staff
This article is a summary / review of the article “Recommendations for the Assessment of Carotid Arterial Plaque by Ultrasound for the Characterization of Atherosclerosis and Evaluation of Cardiovascular Risk: From the American Society of Echocardiography” by Amer M Johri, Vijay Nambi, Tasneem Z Naqvi et al., published June 26, 2020.
See full details here >
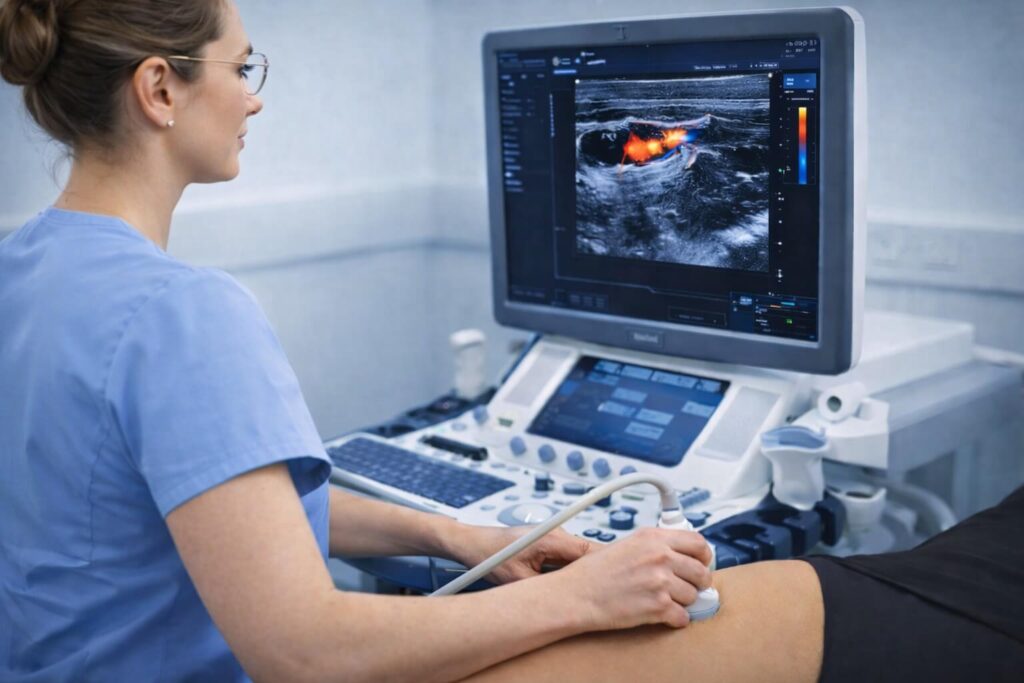
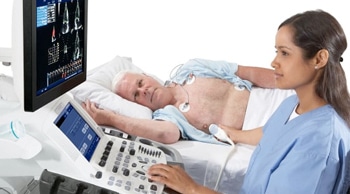
Cardiovascular disease remains a leading cause of death globally, placing a major burden on health care services worldwide. Carotid arteries ultrasound is a first-line imaging able to provide, in a non-invasive way, a unique ‘window’ into the identification of a patient’s underlying cardiovascular risk.
Interest in plaque quantification significantly grew when it was discovered that the presence or absence of plaque conferred additional advantage to risk stratification beyond that provided by carotid intima-media thickness (CIMT) alone (ARIC Study).
Therefore, quantification of carotid arterial plaque has emerged as an important tool for CVD risk stratification as it improve the risk prediction beyond what is provided by cardiovascular risk scores.
Since 2016 the European Society of Cardiology Guidelines on Cardiovascular Disease Prevention has recommended to include plaque detection (carotid arteries plaque and coronary calcium scoring ) as a modifier in cardiovascular risk assessment (class IIb, level B) after the initial assessment performed using established risk scores.
Beyond overall risk stratification, carotid atherosclerosis is also a known predictor of other CVD events, such as stroke resulting from luminal vessel stenosis and plaque rupture.
2020 Recommendations by the American Society of Echocardiography
The recommendations for the assessment of carotid arterial plaque by ultrasound for the characterisation of Atherosclerosis and Evaluation of Cardiovascular Risk, recently published by the American Society of Echocardiography, focuses on the ultrasound methods used to quantify carotid plaque, when present, for the purpose of cardiovascular risk stratification. Emerging techniques, including the role of ultrasound enhancing agents for assessment of intra-plaque neovascularisation and composition analysis, are also discussed in this article alongside with the potential role that 3D ultrasound may play in the evaluation of carotid plaques and cardiovascular risk assessment.
The current document complements the previous consensus article (Stein et al.) in its provision of a standardized approach to defining and quantifying carotid arterial plaque by ultrasound beyond the technical approach to CIMT measurement.
The document illustrates recommendations for subclinical and clinical carotid arteries atherosclerosis.
Carotid intimal-medial thickening (CIMT) is thought to involve thickening of the medial layer whereas plaque is thought to be an intimal process and therefore represents the atherosclerotic process itself. For this reason, carotid plaque and not CIMT has been shown to better predict CVD. As, it can be difficult to discern medial thickening from diffuse atherosclerotic plaque, the Authors have proposed a plaque grading consensus system in order to standardize the size of an individual plaque lesion for the purpose of comparison across studies.
Four grades have been identified:
- Grade 0 – No plaque IMT <1.5 mm
- Grade I – Small protuberant types of plaque lesions with a focal thickening of the vessel wall <1.5 mm, in which currently is not possible to distinguish whether this thickening is entirely due to medial thickening or is intimal
- Grade II – Protuberant or diffuse vessel wall thickened throughout; CIMT >1.5 mm with plaque thickness ranging between 1.5 and 2.4 mm
- Grade III – Protuberant or diffuse vessel wall thickened throughout >2.5 mm
This ultrasound classification of the carotid plaque may help in examining the amount of plaque in order to further personalize a patient’s risk assessment.
This is possible with 2-dimensional (2D) quantification techniques such as the maximal plaque height or thickness, the calculation of the plaque area and even more with the use of the three-dimensional (3D) plaque quantification. The latest allows to measure a specific lesion in all planes thus giving a complete visualization of the plaque geometry, surface and volume.
The recommendations proposed for a standard plaque assessment approach for comparison across studies are the following:
Recommendation #1: Defined carotid arterial plaque visualized by ultrasound (with or without use of an ultrasound enhancing agent [UEA]) in one of the following 2 ways: 1) any focal thickening thought to be atherosclerotic in origin and encroaching into the lumen of any segment of the carotid artery (protuberant-type plaque) or 2) in the case of diffuse vessel wall atherosclerosis, when carotid intima-media thickness (CIMT) measures > 1.5 mm in any segment of the carotid artery (diffuse-type plaque).
Recommendation #2: Evaluate both protuberant and diffuse types of carotid arterial plaque for cardiovascular risk stratification and the serial assessment of atherosclerosis.
Recommendation #3: The carotid arterial wall has to be visually scanned for the presence of protuberant plaque, and if absent, then carotid intima-media thickness (CIMT) measurement has to be performed to identify the presence of diffuse plaque (defined as CIMT >1.5 mm). If performed, CIMT should be measured as described in the ASE Consensus Statement on the Use of Carotid Ultrasound to Identify subclinical Vascular Disease and Evaluate Cardiovascular Risk.
Recommendation #4: Avoid serial carotid intima-media thickness (CIMT) measurements in an asymptomatic patient. Repeat measurements are not recommended unless the Grade and (CIMT) meets criteria for diffuse-type plaque (Grades II or III, and CIMT >1.5 mm) in which case it is a plaque equivalent.
Recommendation #5: Measure plaque thickness (also known as height) as the initial 2-dimensional approach (or 3D when available) for quantification of carotid ultrasound plaque.
Recommendation #6: The maximal plaque height should be measured from the side in which a plaque is detected (unilateral) or from both the right and left carotid arterial segments (bilateral) using a caliper placed at the adventitial plane, and extending into the center of the lumen at right angles to the vessel wall. For the purposes of standardization, this measurement should be taken from any segment of the long and short axis of the carotid artery (bulb, ICA, CCA) and the view and segment re- ported accordingly.
Recommendation #7: Quantify plaque volume for an individual plaque lesion when required (e.g., morphologic assessment, serial assessment, or pre-operative consideration), using either the stacked-contour method or specialized semi-automated tools.
Recommendation #8: Quantify right and/or left carotid arterial plaque volume using 3-dimensional ultrasound for cardiovascular risk stratification.
Recommendation #9: The Authors recommend the single-plaque or single- region protocol where the 3-dimensional volume acquisition is centered over the identified plaque or the right and left carotid arterial bulb, allowing for quantification of total plaque volume in the distal common carotid artery (CCA), bulb, and bifurcation, as well as in the portion of the internal carotid artery (ICA) that can be visualized.
Recommendation #10: A full- vessel protocol has to meet the following criteria: time, expertise, equipment, and analytic software are available for accurate registration of multiple 3-dimensional volume acquisitions. In this latter protocol, total carotid arterial plaque is calculated by summing the volume of plaque seen in all major segments of the right and left carotid arteries.
Translation Into Clinical Practice
Three-dimensional volumetric ultrasound quantification is preferred when available, and a recommendation for plaque volume quantification is provided to promote standardisation. The role of composition analysis to assess plaque vulnerability and tissue types continues to emerge. The important role of plaque analysis by ultrasound in cardiovascular risk stratification continues to require innovative approaches to dissemination of this knowledge and greater efforts toward translation to practice. For primary prevention and/or asymptomatic patients, it appears reasonable to combine established risk scores with plaque
imaging. In the assessment of asymptomatic at-risk patients, the authors suggest a stepwise approach to cardiovascular risk stratification using plaque grading via a focused carotid vascular ultrasound and subsequent 2D or 3D plaque quantification.
Recent studies suggest that carotid plaque imaging in patients with normal stress tests provides improved prognostic information: patients without plaque have an excellent prognosis, whereas patients with a normal imaging test for myocardial ischemia, but atherosclerotic plaques in the carotid artery, may benefit from more aggressive medical treatment.
The combination of carotid plaque assessment with stress testing is a promising area offering enhanced risk stratification. Further multicenter confirmation will allow for consideration of practice recommendations in the future. Monitoring and adjusting treatment of atherosclerosis by repetitive plaque measurements appears to be an attractive application that needs further development of reliable, user friendly tools to assess the carotid plaque burden and clinical studies to define the time intervals and changes in dosing of statins and other medications.
References
Daghem M, Bing R, Fayad ZA, et al. Noninvasive Imaging to Assess Atherosclerotic Plaque Composition and Disease Activity: Coronary and Carotid Applications. JACC Cardiovasc Imaging 2020;13:1055-1068.
Stein JH, Korcarz CE, Hurst RT, Lonn E, Kendall CB, Mohler ER, Najjar SS, Rembold CM, Post WS, American Society of Echocardiography Carotid Intima-Media Thickness Task Force Use of carotid ultrasound to identify subclinical vascular disease and evaluate cardiovascular disease risk: a consensus statement from the American Society of Echocardiography Carotid Intima-Media Thickness Task Force. Endorsed by the Society for Vascular Medicine. J Am Soc Echocardiogr. 2008 Feb;21(2):93-111; quiz 189-90. doi:10.1016/j.echo.2007.11.011. Erratum in: J Am Soc Echocardiogr. 2008 Apr;21(4):376. PMID: 18261694.
Reference For Article Being Summarised / Reviewed
Amer M Johri, Vijay Nambi, Tasneem Z Naqvi, Steven B Feinstein, Esther S H Kim, Margaret M Park, Harald Becher, Henrik Sillesen Recommendations for the Assessment of Carotid Arterial Plaque by Ultrasound for the Characterization of Atherosclerosis and Evaluation of Cardiovascular Risk: From the American Society of Echocardiography J Am Soc Echocardiogr 2020 Aug;33(8):917-933.
Published: June 26, 2020
DOI: 10.1016/j.echo.2020.04.021
Pubmed link >
Journal website with free access to full article >
Keywords: carotid plaque, atherosclerosis, risk stratification