Infrarenal Abdominal Aortic Aneurysm With Chronic Dissection
Discover a case of 74 olders male patient with an abdominal aortic aneurysm (AAA) incidentally detected during an abdominal ultrasound scan requested to assess the liver.
- Abdominal Vessels, Case Studies
- 3 mins

Case study description: Image case study — Infrarenal AAA with chronic dissection
Image case study: No video or audio
This is a case of a 74 years old male patient with an abdominal aortic aneurysm (AAA) incidentally detected during an abdominal ultrasound scan requested to assess the liver. An ultrasound investigation was therefore performed in a specialised vascular laboratory.
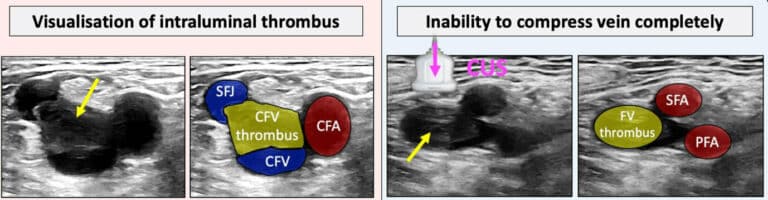
The assessment of the abdominal aorta starts in B-mode transverse view from the epigastric region down towards the iliac bifurcation. The B-mode assessment confirmed the presence of an AAA, with an antero-posterior diameter (AP diameter) of 4.3 cm (figure A). The location of the aneurysm was infrarenal and the shape was fusiform. Moreover, the transverse B-mode view (figure B) also showed an echogenic intimal flap within the aortic lumen. The flap was not mobile and was attached to the medial-posterior wall of the abdominal aorta where chronic mural thrombus was noted. Colour Doppler flow (figure C) was therefore applied and showed a “yin-yang” flow pattern. This is often suggestive of the presence of a true and false lumen and is also present in AAAs. A longitudinal view of the abdominal aorta (figure D) confirmed the presence of a mural thrombus attached to the posterior wall of the abdominal aorta and a chronic dissection arising off this.
An aortic aortic dissection is a condition in which the inner layer of the aorta (intima) tears and blood surges through the tear causing the intima and media layers of the aorta to separate (dissect) creating a false flow lumen. Abdominal aortic dissection is often an extension of a thoracic aorta dissection. Isolated abdominal aortic dissections are rare events. The reported rate of primary abdominal aortic dissection is less than 2%, compared with that of ascending aortic dissection (70%), descending aortic dissection (20%), and aortic arch dissection (7%). In approximately 80% of cases, aortic dissection presents with an acute onset of chest pain that radiates to the back prompting the patient to seek medical care, however, in about 30% of patients, aortic dissection is diagnosed in its chronic state. This is because in a small portion of patient’s symptoms of a chronic aortic dissection can be vague and non-specific, thereby not prompting the patient to seek medical help.
Sonographically, an aortic dissection can be diagnosed by identifying an echogenic intimal flap within the aortic lumen. Aortic dissections can be acute or chronic. In the chronic dissection, the flap often appears echogenic, not mobile with possible calcifications and /or thrombus. In the acute dissection the flap is often mobile and follows the pulsatility of the artery. Colour doppler flow can help to depict both the false and true lumen.
Take home message: Ultrasound is useful in detecting walls abnormalities including aortic dissections, however secondary imaging may be needed to clarify the nature and extension of the aortic dissection.
related courses
Abdominal Aortic Aneurysm Course
Screening for AAA during TTE Course
New Release
Your Ultimate Guide to Carotid plaque Ultrasound Assessment
By: C. Vitale & F. D'Abate
Explore the world of carotid atherosclerotic plaques with ABC Vascular’s latest eBook, “A Practical Guide on the Ultrasound Assessment of Carotid Atherosclerotic Plaques”. This guide offers healthcare professionals a comprehensive understanding of carotid plaque ultrasound assessment and its role in cardiovascular risk management.
Trusted by