Vertebral Artery Hypoplasia: Ultrasound Appearance and Criteria
Explore the ultrasound criteria and appearance of Vertebral Artery Hypoplasia (VAH), a condition often seen in patients with posterior circulation stroke, and understand its clinical implications.
- Articles & Reviews
- 6 mins


March 4, 2020 / / Dr. Cristiana Vitale & ABC Vascular staff
Background
The vertebral arteries, which originate from the subclavian arteries and unite to form the basilar artery after branching into the posterior inferior cerebellar arteries, are the primary blood supply for infratentorial brain structures. Congenital variations in the arrangement and size of the vertebral arteries are common, and vertebral artery hypoplasia (VAH) has frequently been recognised among healthy individuals without symptoms of vertebrobasilar insufficiency.
More recently, several studies have shown that VAH, defined both as a vertebral artery of diameter <2 mm or <3 mm, is commonly observed in patients with posterior circulation stroke. Therefore, it has been speculated that VAH can be associated with an increased probability of ischemic stroke.
However, due to its high prevalence and the lack of a consensual definition of VAH, the clinical significance of VAH as an independent risk factor for ischemic stroke is still debated.
How to Detect Vertebral Artery Hypoplasia With Ultrasound
Definition
The definition of vertebral artery hypoplasia is still unclear, and several criteria have been suggested. Some ultrasound and angiography studies have defined VAH as a vertebral artery with a lumen diameter below 2 mm, while other studies suggest a below 3 mm cut-off diameter.
An asymmetry ratio between vertebral arteries of equal or greater than 1:1.7 has also been suggested to define VAH by other authors. In addition, the measurement of the volume flow within the vertebral arteries has been used as an additional criteria to define VAH with a cut off value of approximately 100 mL/min (see reference by Seidel et al 1999); yet its application in the routine scanning practice seems limited.
“The definition of vertebral artery hypoplasia is still unclear, and several criteria have been suggested”
Ultrasound Assessment
To identify the vertebral artery with ultrasound, a medium-high frequency linear array is generally used; however, a curvilinear array can also be used, in particular when the vertebral arteries lie deep or in presence of short or thick necks.
In order to identify the vertebral artery, the patient generally lies supine on a couch with the head straight or slightly turned towards the opposite side being scanned. The vertebral artery is identified in longitudinal view.
On B-mode, the vertebral artery appears as an anechoic structure that lies between the transverse processes of the cervical spine with the vertebral vein anteriorly (Figure 1).
Figure 1 Description: B-mode longitudinal view image of the vertebral artery (VA) and vertebral vein (VV) lying superiorly to the VA.
Using colour Doppler flow, normally the vertebral artery will present the same colour pattern of the ipsilateral common carotid artery and opposite colour of the one of the vertebral vein.
To measure the diameter of the vertebral artery, an optimal B-mode longitudinal view image is needed. In order to clearly evaluate the lumen of the vertebral artery, focus, time gain compensation, overall B-mode gain and eventually other B-mode parameters should be optimised.
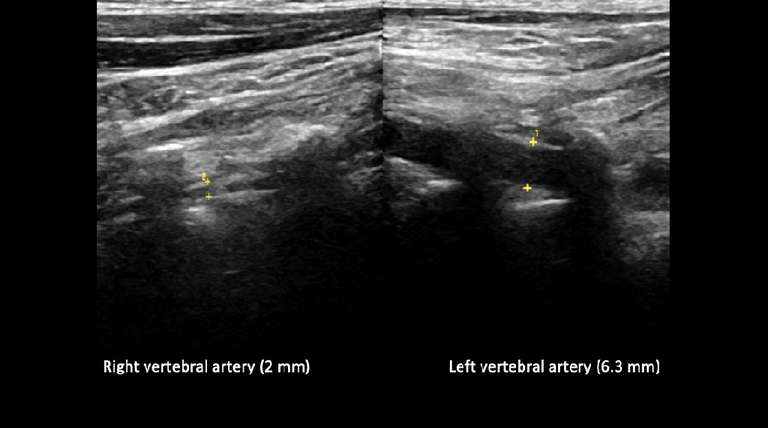
Once the lumen of the vertebral artery is identified the measurement callipers are placed over the outer layer of the posterior and anterior vertebral artery walls (Figure 2). The vertebral artery diameter is generally measured at the V2 level, between the transverse processes of the C4 and C5 vertebra.
Figure 2 Description: B-mode longitudinal view of the right and left vertebral artery and the respective diameters measured with callipers measurements. In the right panel the right vertebral artery diameter measures 2 mm (2) while on the left panel the left vertebral artery measures 6.3 mm (1). Additionally, the asymmetry ratio in this particular case is 1:3.15.
Pulsed wave Doppler waveforms are also used as an additional criterion to define VAH. A normal vertebral artery presents antegrade low resistance Doppler flow pattern with a pronounced diastolic component. In presence of VAH the Doppler flow waveform changes with a less pronounced diastolic component reflecting the higher resistance, caused by the smaller diameter.
Complete absence of the diastolic flow and a low peak systolic flow velocity can be suggestive of distal intracranial steno-obstructive disease; therefore, further imaging is usually suggested in these circumstances.
In presence of VAH, the diastolic flow is generally represented even if of small amplitude. As shown in figure 2, while the left (dominant artery) vertebral artery presents a normal low resistance Doppler waveform, the right vertebral artery presents a high resistance pattern with a low diastolic flow.
Figure 3 Description: Pulsed wave Doppler flow analysis throughout the right (VAH) and left (dominant) vertebral arteries. High resistance flow is noted in the right vertebral artery with small diastolic component shown on the Doppler trace. The left vertebral artery presents a normal antegrade low resistance Doppler flow with pronounced diastolic component.
Conclusion
Despite the lack of consensus on diagnostic criteria to define VAH, the most commonly used are:
- Diameter of the vertebral artery < 2 mm or < 3 mm
- An asymmetry ratio between vertebral arteries of equal or greater than 1:1.7
- Volume flow within the vertebral artery < 100 mL/min.
“The most commonly used criteria for VAH (Vertebral Artery Hypoplasia) are:
– Diameter of the vertebral artery < 2 mm or < 3 mm
– An asymmetry ratio between vertebral arteries of equal or greater than 1:1.7
– Volume flow within the vertebral artery < 100 mL/min.”
Related ABC Vascular Courses
Have you considered learning more with these related courses?
Master course on Carotid and Vertebral Arteries
Info on the “Carotid and Vertebral Arteries” course >
Short course on How to Diagnose Subclavian Steal Syndrome (SSS)
More on the “How to Diagnose Subclavian Steal Syndrome” course >
Additional Reading
Katsanos AH, Kosmidou M, Kyritsis AP, Giannopoulos S. Is Vertebral Artery Hypoplasia a Predisposing Factor for Posterior Circulation Cerebral Ischemic Events? A Comprehensive Review. Eur Neurol. 2013;70(1-2):78–83. https://www.ncbi.nlm.nih.gov/pubmed/23816871
Perren F, Poglia D, Landis T, Sztajzel R. Vertebral artery hypoplasia: A predisposing factor for posterior circulation stroke? Neurology. 2007;68(1):65–7. https://www.ncbi.nlm.nih.gov/pubmed/17200496
E. Seidel, B.M. Eicke, B. Tettenborn, F. Krummenauer Reference Values for Vertebral Artery Flow Volume by Duplex Sonography in Young and Elderly Adults. Stroke 1999; Dec;30(12):2692-6. https://www.ahajournals.org/doi/pdf/10.1161/01.STR.30.12.2692
Chuang YM, Chan L, Wu HM, Lee SP, Chu YT. The clinical relevance of vertebral artery hypoplasia. Acta Neurol Taiwan. 2012 Mar;21(1):1. https://www.ncbi.nlm.nih.gov/pubmed/22879083
Chi HY, Chen KW, Hsu CF, Shen CY, Chen AC, Su C, Fu WM Ultrasound Findings Disclose the Mutual Impact of Vertebrobasilar Dolichoectasia and Vertebral Artery Hypoplasia. J Ultrasound Med. 2019 Nov;38(11):3037-3042. https://onlinelibrary.wiley.com/doi/abs/10.1002/jum.15011
Kulyk C, Voltan C, Simonetto M, Palmieri A, Farina F, Vodret F, Viaro F, Baracchini C. Vertebral artery hypoplasia: an innocent lamb or a disguise? J Neurol. 2018 Oct. https://www.ncbi.nlm.nih.gov/pubmed/30116939

related courses
Carotid Ultrasound Course and Vertebral Arteries
Corso Imaging Ultrasonografico dell’Aneurisma dell’Aorta Addominale
Evaluación de la Placa Aterosclerótica Carotídea
Carotid Atherosclerotic Plaque Assessment Course
Lower Limb Venous System Course
Abdominal Aortic Aneurysm Course
Screening for AAA during TTE Course
Como Diagnosticar Trombosis Venosa Profunda Poplítea Femoral + CME Quiz
How to Diagnose Subclavian Steal Syndrome Course + CME Quiz
How to Diagnose a Femoral-Popliteal DVT Course + CME Quiz
New Release
Your Ultimate Guide to Carotid plaque Ultrasound Assessment
By: C. Vitale & F. D'Abate
Explore the world of carotid atherosclerotic plaques with ABC Vascular’s latest eBook, “A Practical Guide on the Ultrasound Assessment of Carotid Atherosclerotic Plaques”. This guide offers healthcare professionals a comprehensive understanding of carotid plaque ultrasound assessment and its role in cardiovascular risk management.
Trusted by